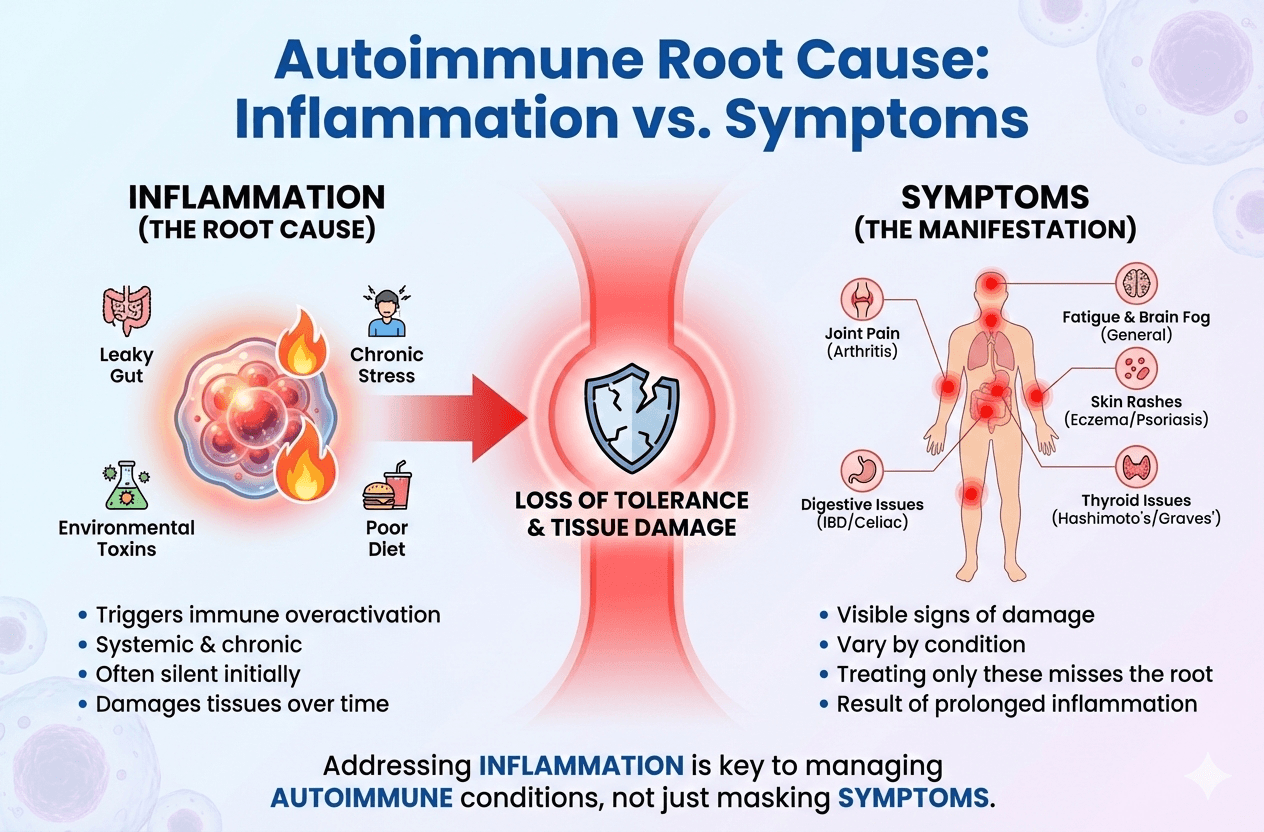
Autoimmune Root Cause: Inflammation vs. Symptoms

What if your autoimmune disease is actually a metabolic inflammation problem?
For millions living with autoimmune conditions, from Hashimoto's thyroiditis to rheumatoid arthritis to lupus, the conventional medical narrative is frustratingly simple: your immune system has gone haywire and is attacking your own tissues. The standard solution usually involves suppressing the immune response with medications, managing symptoms as they arise, and accepting a lifetime of pharmaceutical intervention.
But this framework treats autoimmune disease as the root problem rather than the symptom. What if we've been looking at this backward? What if many autoimmune conditions aren't isolated immune system failures, but rather downstream consequences of chronic metabolic inflammation—a systemic fire that's been burning quietly for years before your body finally raises the alarm?
This reframing isn't just a matter of semantics. It fundamentally changes how we understand, manage, and support our bodies through autoimmune and metabolic dysfunction.
Act 1: The Inflammation-Immune-Metabolism Triangle
The Conventional Model's Blind Spot
Conventional autoimmune treatment operates on a straightforward premise: if the immune system is attacking healthy tissue, suppress immune function until the attack stops. Medications like corticosteroids, disease-modifying antirheumatic drugs (DMARDs), and biologics all work by dampening immune responses.
This approach often reduces symptoms, at least temporarily, and is a crucial part of acute care. But it rarely addresses why the immune system became dysregulated in the first place. It's like disconnecting your car's check engine light instead of fixing the engine. The warning stops, but the underlying wear and tear accelerates.
The critical insight emerging from metabolic and immunological research is this: chronic inflammation is both the trigger and the sustainer of autoimmune dysfunction.
How Inflammation Hijacks Immunity
Inflammation is supposed to be acute and self-limiting, a short-term, healthy response to injury or infection. When you cut your finger, inflammatory signals recruit immune cells, clear debris, and initiate healing. Then, the inflammation resolves.
However, chronic, low-grade inflammation operates differently. It creates a state of persistent immune activation, where inflammatory signaling molecules (cytokines) remain elevated for months or years. According to the National Institutes of Health (NIH), this chronic signaling disrupts the body in several distinct ways:
- Confuses immune tolerance: The constant inflammatory noise makes it harder for your immune system to distinguish "self" from "foreign." Molecular mimicry, where inflamed human tissues start resembling pathogens, becomes more likely.
- Exhausts regulatory cells: T-regulatory cells (Tregs) that normally act as the "brakes" to prevent autoimmune attacks become depleted or dysfunctional under chronic inflammatory stress.
- Increases tissue permeability: Chronic inflammation damages barrier tissues (like the gut lining or blood-brain barrier), allowing undigested proteins and bacterial fragments into circulation where they trigger systemic immune responses.
- Creates oxidative stress: Inflammatory processes generate reactive oxygen species that damage cellular components, creating debris that the immune system must continuously clear, perpetuating an endless cycle.
The Metabolic Connection
Here's where the model gets even more revealing: the exact same chronic inflammation that drives autoimmunity also causes metabolic dysfunction.
Inflammatory cytokines directly interfere with insulin signaling, contributing to insulin resistance. They disrupt mitochondrial function, reducing your cellular energy production. They alter lipid metabolism, promoting fat storage and making weight loss incredibly difficult. They even dysregulate hunger hormones, leading to cravings and overeating.
This explains why autoimmune conditions so often cluster with metabolic issues:
- Hashimoto's thyroiditis frequently accompanies insulin resistance and weight gain.
- Psoriasis correlates strongly with metabolic syndrome.
- Lupus patients often show higher rates of cardiovascular disease and blood sugar imbalances.
- Rheumatoid arthritis is frequently associated with dyslipidemia and stubborn weight retention.
These aren't entirely separate diseases, they are often different physical manifestations of the exact same underlying inflammatory state.
Act 2: The Modern Inflammatory Storm
What's Fueling Chronic Inflammation?
If chronic inflammation is the root cause, what is causing the inflammation in the first place? The answer largely lies in the profound mismatch between our ancestral biology and our modern environment.
1. The Industrial Diet
Heavily processed foods create multiple inflammatory pathways in the body.
- Omega-6/Omega-3 imbalance: Modern diets contain 15 to 20 times more omega-6 fatty acids (from seed oils and grain-fed meat) than anti-inflammatory omega-3s.
- Advanced glycation end products (AGEs): These inflammatory compounds form when sugars react with proteins or fats, especially during high-heat cooking.
- Refined carbohydrates and sugar: Rapid blood sugar spikes stimulate heavy insulin release. This creates a vicious cycle of insulin resistance, higher insulin levels, and widespread inflammation.
- Emulsifiers and additives: Common modern food additives can disrupt the protective gut mucus layer, increasing intestinal permeability.
2. Environmental Toxins
We are exposed to thousands of synthetic chemicals that didn't exist a century ago. Endocrine disruptors (like BPA and phthalates) interfere with hormone signaling and immune function. Many of these accumulate in fatty tissue. Heavy metals create oxidative stress, and air pollution generates systemic inflammation through particulate matter that crosses from the lungs into the bloodstream.
3. Chronic Stress and Cortisol Dysregulation
The human stress response is designed for acute, short-term threats. Cortisol helps mobilize energy and temporarily suppresses inflammation so you can survive a crisis. But chronic psychological stress (financial pressure, relationship strain, constant work demands) keeps cortisol elevated indefinitely.
Initially, high cortisol is anti-inflammatory. But over time, your cells become resistant to cortisol's signals. When this happens, inflammatory pathways run unchecked even while cortisol remains high. You get the worst of both worlds: stress hormone damage plus uncontrolled inflammation.
4. Sleep Deprivation and Circadian Disruption
Sleep is when the body performs essential cellular cleanup and immune recalibration. The Centers for Disease Control and Prevention (CDC) routinely highlights that chronic sleep restriction is linked to severe chronic diseases. Lack of sleep impairs glucose metabolism, reduces natural killer cell activity, and increases inflammatory markers within days.
5. Microbiome Destruction
Your gut contains trillions of bacteria that regulate immune function, produce anti-inflammatory compounds, and maintain intestinal barrier integrity. When beneficial bacteria decline due to antibiotics, low-fiber diets, or chronic stress, opportunistic inflammatory species proliferate, causing "leaky gut" and systemic immune responses.
Act 3: The Inflammation-First Approach
Why Treating Inflammation Transforms Both Conditions
If chronic inflammation drives both autoimmune and metabolic dysfunction, then targeting inflammation directly should improve both simultaneously. And that is exactly what modern research demonstrates.
- Dietary Interventions: Anti-inflammatory diets (like the Mediterranean diet or Autoimmune Protocol) consistently show improvements in both autoimmune markers and metabolic parameters. Patients frequently report reduced joint pain, better blood sugar control, and weight loss from the exact same dietary shift.
- Strategic Exercise: Consistent, moderate exercise reduces inflammatory cytokines while improving insulin sensitivity. (The key is avoiding overtraining, which can trigger inflammatory stress).
- Stress Management: Practices like meditation, breathwork, or therapy reduce cortisol dysregulation.
- Sleep Optimization: Improving sleep quality has systemic effects that rival pharmacological interventions for reducing inflammation.
The Clustering Phenomenon
The inflammation model elegantly explains why autoimmune conditions and metabolic issues cluster together, and why people with one autoimmune condition often develop others. It isn't just "bad luck", it's the same inflammatory fire spreading to different tissues.
Your unique genetic vulnerabilities determine which tissues fail first under inflammatory stress. One person develops thyroid antibodies, another gets joint inflammation, and another experiences skin manifestations. But the root driver, chronic inflammation, is shared.
Reframing Treatment Strategy
Viewing autoimmune disease through the lens of metabolic inflammation shifts your daily health priorities:
- Step 1: Identify and remove inflammatory dietary and environmental triggers.
- Step 2: Restore metabolic flexibility through nutrient-dense whole foods and optimized sleep.
- Step 3: Heal barrier tissues (like the gut lining) to reduce inappropriate immune exposure.
- Step 4: Address root causes (chronic stress, poor microbiome health) rather than just managing symptoms.
This doesn't mean abandoning conventional treatment. Severe autoimmune flares require diligent medical management. But it means recognizing that symptom suppression is only one half of the healing equation.
Maryland Trim Clinic (MTC) in Laurel, MD
If you are struggling with the frustrating overlap of metabolic dysfunction, weight retention, and systemic inflammation, the Maryland Trim Clinic (MTC) in Laurel, MD, offers supportive, science-backed care. Managing the root causes of inflammation requires more than just willpower; it requires understanding exactly how your unique body is functioning.
The dedicated team at MTC helps patients uncover the biological roadblocks preventing them from feeling their best. By utilizing tools like metabolic testing and analysis, they can identify hidden inefficiencies in your body's energy production. From there, they offer personalized nutritional counseling and coaching to help you adopt a sustainable, anti-inflammatory lifestyle, or a comprehensive medical weight loss program to address the metabolic side of the equation. By addressing the root causes of systemic stress, MTC partners with you to build a foundation for long-term vitality.
Conclusion
Your autoimmune diagnosis may be real, but it is likely not the foundational problem, it is your body's alarm system responding to chronic metabolic inflammation. The exact same inflammatory processes that confuse your immune system are also disrupting your metabolism, energy production, weight regulation, and cardiovascular health.
This explains why autoimmune and metabolic conditions cluster together, why conventional treatments often fail to address the full picture, and why comprehensive anti-inflammatory interventions can transform your health so profoundly.
The question isn't whether your autoimmune disease is "real", your symptoms and suffering are absolutely valid. The question is: what if managing inflammation as the primary problem is the key to unlocking a better quality of life? For many, that reframing is the difference between lifelong frustration and genuine, holistic improvement.
Medical Disclaimer: The information provided in this article is for educational and informational purposes only and is not intended as medical advice. Always consult with a qualified healthcare provider before making any changes to your diet, lifestyle, or medication regimen, especially if you have been diagnosed with an autoimmune or metabolic condition.
Frequently Asked Questions
Q: Is autoimmune disease the same as chronic inflammation? A: Autoimmune disease is typically a consequence of chronic inflammation rather than being identical to it. Chronic inflammation creates the environment that leads to immune dysregulation, it confuses immune tolerance, damages barrier tissues, and creates oxidative stress. The autoimmune condition is the downstream result.
Q: Can addressing inflammation reverse autoimmune disease? A: While results vary greatly by individual and disease severity, many people experience significant symptom improvement or clinical remission by addressing chronic inflammation through diet, lifestyle, and stress management. However, this doesn't mean abandoning medical care, severe cases always require professional medical management.
Q: Why do autoimmune conditions often come with weight gain and metabolic problems? A: The same inflammatory cytokines that drive autoimmune responses also disrupt metabolic function. Inflammation interferes with insulin signaling (causing insulin resistance), disrupts mitochondrial function, alters hunger hormones, and promotes fat storage.
Q: What are the most important lifestyle changes to reduce inflammation? A: The most impactful changes include:
- Adopting an anti-inflammatory diet (eliminating ultra-processed foods, increasing omega-3s).
- Optimizing sleep quantity and quality (7-9 hours consistently).
- Managing chronic stress through meditation or therapy.
- Engaging in regular moderate exercise without overtraining.
- Supporting gut health with fiber and fermented foods.
Q: How long does it take to see improvements from an anti-inflammatory approach? A: The timeline varies significantly. Some people notice improvements in daily energy and joint pain within 2 to 4 weeks of dietary changes. More substantial changes in autoimmune markers and metabolic function typically require 3 to 6 months of consistent intervention and lifestyle adjustments.
Ready to Address Your Metabolic Health?
Take the First Step Toward Lower Inflammation Today Stop fighting your body and start supporting it. If you're ready to explore how managing your metabolic health can improve your quality of life, reach out to the experts. Visit Maryland Trim Clinic online to schedule a consultation and begin your personalized wellness journey.