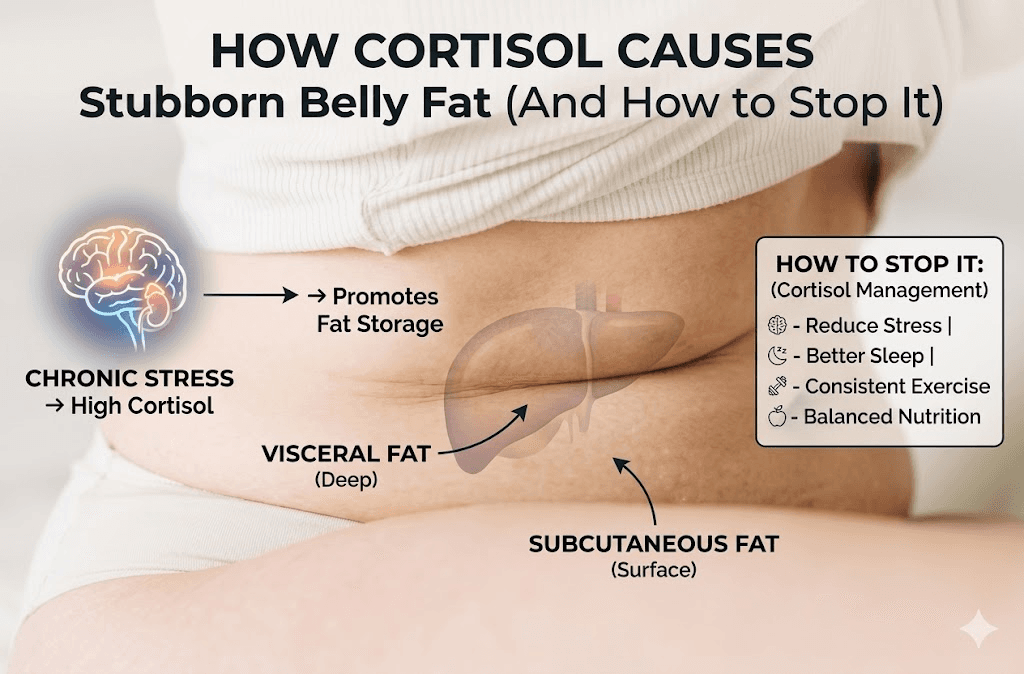
How Cortisol Causes Stubborn Belly Fat (And How to Stop It)

Your stress is making you hold onto weight, and no workout can out-train high cortisol.
If you are exercising regularly, eating reasonably well, and still watching your waistline expand, you are not failing. You are fighting a biological battle you were likely never told about. The real enemy isn't simply "calories in versus calories out." It is a stress hormone called cortisol, and when it is chronically elevated, it fundamentally rewires your body's fat storage system to prioritize one place above all others: your abdomen.
This is not a motivational problem. This is a physiological problem—and understanding the mechanism is the first step to reversing it safely.
ACT 1: What Cortisol Actually Does to Your Body Fat
The Hormone Your Body Uses in Emergencies
Cortisol is produced by the adrenal glands in response to stress. This applies to any stress, whether that is a looming work deadline, a poor night of sleep, a difficult relationship, financial pressure, or even an intensely grueling workout. In short bursts, cortisol is life-saving. It mobilizes energy, sharpens focus, and prepares your body to respond to an immediate threat.
The problem is that modern life does not give cortisol a natural off-switch.
When stress becomes chronic, cortisol levels stay elevated for hours and days at a time rather than spiking and falling within minutes. That sustained elevation triggers a cascade of metabolic consequences specifically designed—from an evolutionary standpoint—to keep you alive during prolonged hardship. Unfortunately, those same survival mechanisms translate directly into stubborn belly fat in the 21st century.
Why Fat Goes Straight to Your Belly
Visceral fat—the deep abdominal fat that surrounds your internal organs—is not just cosmetically frustrating. It is metabolically active, hormonally disruptive, and directly linked to an increased risk of cardiovascular disease and type 2 diabetes.
According to peer-reviewed research published by the National Institutes of Health (NIH), visceral fat has a particular affinity for cortisol. Visceral fat cells have a significantly higher concentration of glucocorticoid receptors than subcutaneous fat (the soft fat just under your skin). When cortisol binds to these receptors in your belly, it does two critical things:
It amplifies the signal: It activates an enzyme (11β-HSD1) that actually regenerates cortisol locally within the fat cells.
It multiplies fat cells: It increases the size and number of visceral fat cells by prompting early-stage fat cells to mature in the abdominal region.
In plain terms: cortisol tells your belly fat to grow, and your belly fat has more receptors to "hear" that message than anywhere else on your body. For individuals struggling to correct these profound hormonal imbalances, specialized interventions like hormone replacement therapy can sometimes provide the necessary foundation for recovery.
The Insulin Resistance Loop
Cortisol does not work in isolation. It also raises blood glucose by stimulating your liver to produce emergency fuel. This chronically elevated blood sugar triggers repeated insulin spikes. Over time, your cells become resistant to insulin's signal, leaving both blood sugar and insulin levels chronically high. Because insulin is one of the most powerful fat-storage signals in the human body, it works synergistically with cortisol to lock fat into the abdominal region.
The Muscle-Wasting Component
Cortisol is also catabolic—meaning it breaks down tissue for fuel. Under chronic stress, it preferentially breaks down lean muscle mass. Less muscle means a slower resting metabolic rate, causing you to burn fewer calories at rest. The cruel irony is that as cortisol destroys muscle and packs on visceral fat, your metabolism slows, making future fat loss even harder.
ACT 2: Why Your Workouts Might Be Making Things Worse
The Exercise Cortisol Spike
Exercise is a physiological stressor. That is not inherently a bad thing; acute exercise-induced cortisol spikes are part of what makes training effective. Under normal hormonal conditions, you work out, cortisol rises briefly, the workout ends, cortisol falls, and the body recovers and rebuilds stronger.
But here is where it breaks down for chronically stressed individuals: if your cortisol baseline is already elevated before you even lace up your shoes, adding a high-intensity workout stacks another massive cortisol spike onto an already dysregulated system. Your body never gets a true recovery window. The fat-storing signal stays glued to the "on" position.
High-Intensity Training and the Overtraining Trap
High-intensity interval training (HIIT), heavy lifting, and long-duration cardio sessions—the exercise modalities most commonly pushed by fitness culture for fat loss—produce the largest cortisol responses.
For someone well-rested and managing stress effectively, these are powerful tools. But for someone who is sleeping six hours a night, skipping meals, managing a high-pressure job, and metabolically stressed, these workouts can actively impede fat loss. Studies show that chronically stressed individuals performing high-intensity exercise experience impaired muscle recovery and a paradoxically increased appetite. You work harder, eat more, store more fat, and lose more muscle.
Quick Swaps for Stressed Bodies
If you feel constantly drained but the scale won't budge, it's time to swap your routine:
- If you currently do: 5 days of intense HIIT classes.
- Try swapping to: 2 days of moderate strength training and 3 days of Zone 2 cardio (brisk walking or light cycling).
- If you currently do: Long, grueling 90-minute runs.
- Try swapping to: 45 minutes of Pilates, yoga, or swimming.
- If you currently feel: Exhausted after a workout rather than energized.
- Try swapping to: Active recovery days focused entirely on mobility and stretching until your energy baseline returns.
ACT 3: How to Actually Lower Cortisol and Lose the Belly Fat
The good news is that the cortisol-belly fat cycle is highly reversible. It requires a multi-pronged approach that targets the stress response system directly. Here is a medically sound framework to guide you:
1. Prioritize Sleep Above Everything Else
Sleep is the single most powerful cortisol-regulating intervention available. According to the Centers for Disease Control and Prevention (CDC), adults require 7 or more hours of sleep per night for optimal metabolic and immune function. Chronic sleep deprivation of six hours or less is one of the strongest predictors of elevated cortisol and visceral fat accumulation.
- Action Step: Eliminate blue light exposure 60 to 90 minutes before bed and keep the bedroom cool (between 65–68°F) to support deep, restorative sleep architecture.
2. Leverage Evidence-Based Supplements (With Doctor Approval)
Certain vitamins and minerals have clinical evidence supporting their role in cortisol regulation:
- Magnesium: Magnesium deficiency directly impairs the brain's ability to shut down the stress response. Magnesium glycinate (300–400 mg in the evening) can support sleep quality and calm the nervous system.
- Ashwagandha: This adaptogenic root has strong clinical evidence for reducing serum cortisol and fasting blood glucose when used consistently for 60 days.
- Vitamin C: The adrenal glands require dense amounts of vitamin C to regulate cortisol. High-dose vitamin C can help blunt the cortisol spike following intense exercise. (Always consult your physician before starting any new supplement regimen to ensure it is safe for your specific health profile.)
3. Regulate Blood Sugar to Break the Cycle
Because cortisol and insulin work together to drive visceral fat, stabilizing blood sugar is critical. Working with professionals through structured nutritional counseling and coaching can help you build a diet that prevents spikes and crashes.
- Action Step: Eat high-quality protein and healthy fats with every meal to slow glucose absorption, and avoid skipping meals, as low blood sugar is itself a primary cortisol trigger.
4. Implement Nervous System Regulation
The autonomic nervous system is the upstream regulator of cortisol. Shifting into "rest-and-digest" (parasympathetic) mode is one of the fastest ways to lower cortisol in real time.
- Action Step: Practice 4-7-8 breathing (inhale for 4 counts, hold for 7, exhale for 8) for just 5 minutes a day to activate the vagus nerve and pull the body out of fight-or-flight mode.
Maryland Trim Clinic (MTC) in Laurel, MD
Reversing stubborn, stress-induced weight gain requires more than just trying harder—it requires a precise, medically supervised strategy that addresses your unique biology. Located in Laurel, MD, the Maryland Trim Clinic (MTC) provides a comprehensive, compassionate environment where patients can finally address the root hormonal causes of their weight struggles.
When standard diet and exercise are no longer working due to metabolic or stress-related roadblocks, MTC's tailored medical weight loss program can help. By utilizing advanced diagnostics, evidence-based therapies, and holistic lifestyle coaching, the clinical team at MTC works with you to balance your hormones, lower systemic stress, and gently guide your body back to a state where sustainable fat loss is actually possible.
The Bottom Line
Belly fat in chronically stressed adults is not a willpower problem. It is a hormonal problem with a specific mechanism and, critically, specific solutions. Cortisol acts directly on visceral fat cells, drives insulin resistance, breaks down muscle, and creates an internal environment where fat loss becomes physiologically impaired.
The path forward is not to push harder. It is to work smarter by addressing the hormonal root cause through targeted nutrition, strategic exercise, and genuine recovery. You do not have a discipline problem. You have a cortisol problem. And with the right medical and lifestyle tools, you can fix it.
Medical Disclaimer: The information provided in this article is for educational purposes only and is not intended as a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician regarding a medical condition, treatment options, or before altering your prescribed health routine.
FAQs
Why does stress specifically cause belly fat and not fat in other areas? Visceral fat cells in the abdominal region have a much higher concentration of glucocorticoid receptors than fat cells elsewhere. These receptors are specifically activated by cortisol. Furthermore, a local enzyme actually regenerates cortisol within those specific fat cells, amplifying the fat-storage signal right in your midsection.
Can I still do high-intensity workouts if I have high cortisol? You do not have to eliminate high-intensity exercise entirely, but frequency matters significantly. Limiting HIIT or heavy training to one or two sessions per week, and filling the remaining days with moderate Zone 2 cardio (like brisk walking) is a much smarter strategy when your body is under high chronic stress.
How long does it take to see results from lowering cortisol? Cortisol regulation can begin showing measurable improvements in sleep and energy within two to four weeks of consistent intervention. Visible changes in visceral fat, however, may take 8–12 weeks, as this type of fat is metabolically stubborn even when cortisol is being addressed properly.
What is the best supplement to start with for high cortisol? Magnesium is the most accessible starting point for most people, given how widespread deficiency is and its direct role in regulating the stress axis and sleep quality. Magnesium glycinate taken in the evening is highly recommended. Always verify with your doctor before starting.
Does cortisol-driven belly fat affect women over 40 differently? Yes. During perimenopause and menopause, declining estrogen levels remove a key hormonal buffer against cortisol's fat-storing effects. As estrogen falls, visceral fat cells become even more responsive to cortisol, which is why many women notice sudden abdominal fat gain in their 40s despite no changes in diet or activity.
Does skipping meals or intermittent fasting raise cortisol? Yes. Prolonged fasting or meal skipping can trigger cortisol release, as the body interprets low blood glucose as a physiological stressor. For individuals with already-elevated cortisol, aggressive intermittent fasting can worsen hormonal dysregulation. A more cortisol-friendly approach is to eat balanced meals at regular intervals.
Ready to Finally Lose That Stubborn Belly Fat?
Stop fighting a losing battle against your own hormones. Visit the Maryland Trim Clinic homepage today to schedule a consultation. Our expert medical team in Laurel, MD, is ready to help you lower your stress, balance your metabolism, and build a weight loss plan that actually works for your body.