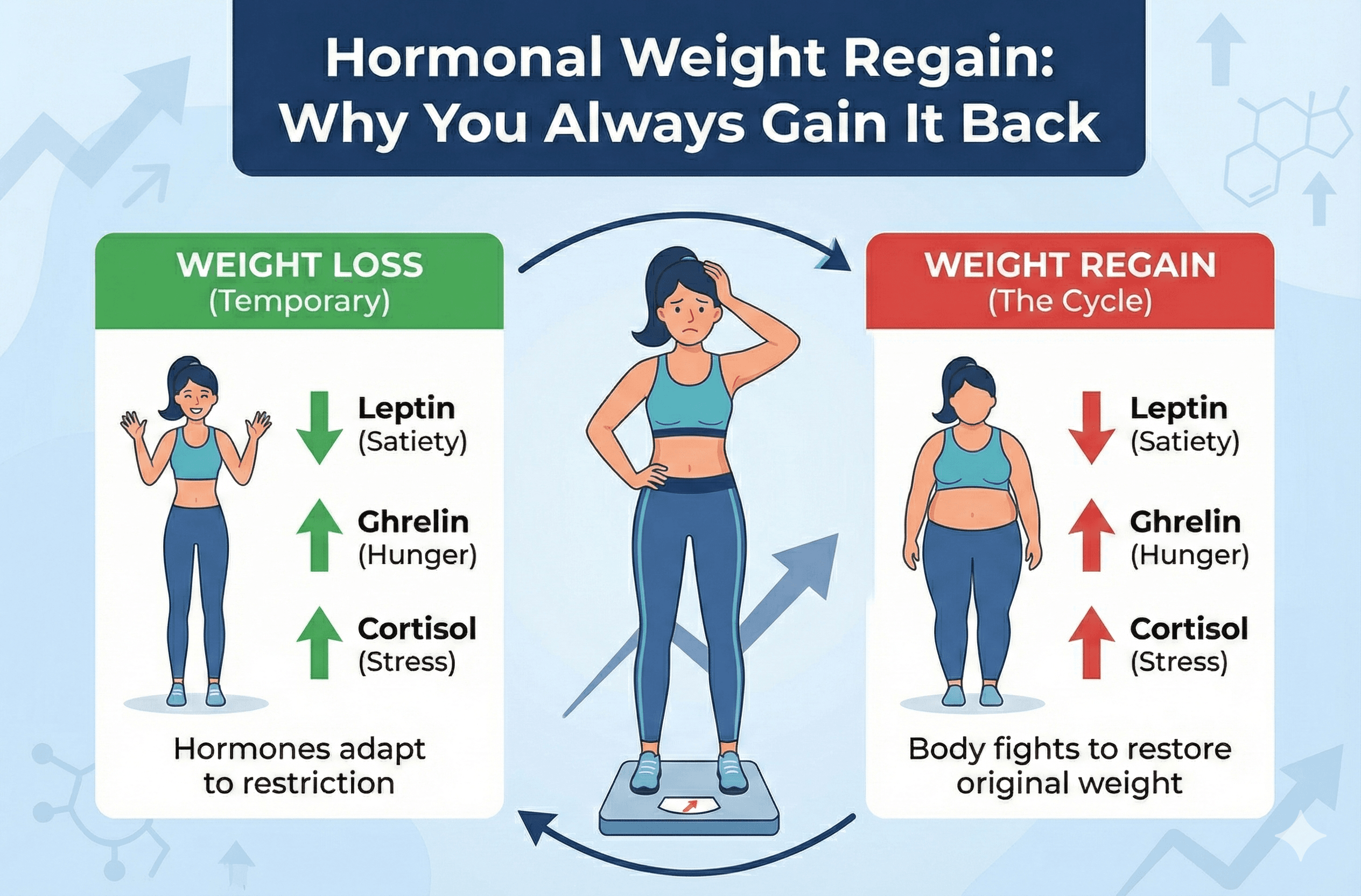
Hormonal Weight Regain: Why You Always Gain It Back

It's not willpower, your hormones are biologically programmed to make you regain weight. Here's the science.
You've been here before. The new diet works brilliantly at first. The pounds melt off, your clothes fit better, and you feel entirely in control. Then, slowly, or sometimes suddenly, the weight creeps back.
When this happens, you likely blame yourself. You assume you lacked discipline, gave in to temptation, or simply weren't strong enough to stick it out. But the real culprit isn't your willpower. It's your hormones.
Your body operates a highly sophisticated biological system designed to defend your body weight at all costs. When you lose weight, this system activates aggressive compensatory mechanisms that increase your hunger, reduce your metabolism, and fundamentally alter how your brain perceives food.
Understanding these hormonal changes isn't about making excuses for weight gain, it's about recognizing that serial dieters are fighting a grueling uphill battle against millions of years of evolutionary programming. The good news? Once you understand the internal machinery driving weight regain, you can finally work with it instead of against it.
ACT 1: The Hormonal Perfect Storm
When you lose weight, your body doesn't know you are trying to look good for a vacation or improve your blood pressure. It thinks you are starving. Consequently, it alters three major hormones to save your life.
Leptin: The Satiety Signal That Disappears
Leptin is a hormone produced by your fat cells. It acts as your body's satiety signal. Think of it as the "I'm full" message sent directly to your brain. When you have adequate fat stores, leptin circulates in your bloodstream, telling your hypothalamus that you have sufficient energy reserves and do not need to eat.
But here is the problem: when you lose weight, your fat cells shrink, and leptin production plummets. A landmark study published by the National Institutes of Health (NIH) followed contestants from The Biggest Loser and found that six years after their dramatic weight loss, their leptin levels remained significantly suppressed—often at only 60% of the expected levels for their current weight.
This leptin deficiency has cascading, devastating effects on a diet. Your brain interprets low leptin as starvation, regardless of how many calories you actually ate that day. This triggers a biological alarm system that makes food seem more rewarding, increases food-seeking behavior, and drastically reduces the physical satisfaction you get from eating a meal. You are literally fighting a brain that believes you are dying of starvation.
Ghrelin: The Hunger Hormone on Overdrive
If leptin is the brake pedal on your appetite, ghrelin is the accelerator, and after weight loss, your body presses it to the floor.
Ghrelin is produced primarily in your stomach. It surges before meals, creating the physical sensation of a grumbling, empty stomach. Normally, ghrelin levels drop after you eat, signaling satisfaction.
However, after sustained weight loss, ghrelin production increases dramatically and stays elevated. Research shows that successful dieters experience ghrelin levels up to 24% higher than before they lost the weight, even a full year later.
The ghrelin-leptin combination is particularly insidious:
- Low leptin removes the brake (you never feel full).
- High ghrelin slams the accelerator (you feel constantly starving).
Your appetite isn't just elevated; it is in a constant state of emergency.
Insulin: The Fat Storage Switch
Insulin's primary job is regulating blood sugar, but it also plays a crucial role in fat storage. After cycles of yo-yo dieting and weight regain, many people develop or worsen insulin resistance, a condition where cells become "numb" to insulin's signals.
This creates two massive roadblocks for weight maintenance:
Your pancreas must produce more insulin to do the same job, keeping insulin levels chronically elevated in your bloodstream. High insulin directly promotes fat storage and chemically blocks fat breakdown.
Insulin resistance in the brain disrupts hunger signaling and reward processing.
When you combine missing leptin, surging ghrelin, and insulin dysfunction, you create a physiological environment where your body is biochemically driven to regain weight. It's not a character flaw. It is biology.
ACT 2: Your Brain's Set Point Defense System
Hormones drive the hunger, but your metabolism determines how the calories are used.
Metabolic Adaptation: The Efficiency Curse
Your body responds to weight loss by becoming metabolically hyper-efficient, meaning it burns fewer calories at rest than would normally be predicted for your new, smaller body size. This phenomenon is called "adaptive thermogenesis" or "metabolic adaptation," and it can persist for years.
In the Biggest Loser study, contestants were burning an average of 500 fewer calories per day than expected for people of their size, even six years post-show. This wasn't because they stopped exercising; their resting metabolic rate had fundamentally downshifted. Their bodies had permanently adjusted to defend against any further weight loss.
This metabolic slowdown compounds your hormonal hunger. You are not only hungrier, but you also require fewer calories to maintain your weight than someone who has always been that size. The caloric deficit required to maintain your weight loss becomes increasingly, agonizingly unsustainable.
Brain Insulin Resistance: The Willpower Myth
Recent research has identified insulin resistance specifically in the brain as a key driver of weight regain. The hypothalamus, which regulates energy expenditure, depends on insulin signaling to gauge your energy status. When brain insulin resistance develops, this signaling becomes totally distorted.
Functional MRI studies show that after weight loss, the brain's reward centers light up intensely in response to high-calorie foods, while activity in the prefrontal cortex (the rational, self-control center) actually diminishes. This is not a willpower failure, it is a neurological shift. Your logical brain is literally fighting a losing battle against a hypothalamus screaming for dense calories.
The Set Point: Your Body's Defended Territory
Your body appears to fiercely defend a "set point", a specific weight range it considers normal, safe, and necessary for survival. This set point is influenced by:
- Your genetics.
- Your metabolic history.
- The highest weight you have ever maintained for an extended period.
When you drop below this range, your body activates every hormonal and metabolic tool in its arsenal to pull you back up. Evolutionarily, this made perfect sense; a body that defended against weight loss survived famines. But in a modern environment where ultra-processed food is cheap and abundant, this ancient survival system guarantees rapid weight regain.
ACT 3: Working With Biology, Not Against It
If willpower can't beat biology, what can?
Medical Interventions That Address Hormones
The most promising developments in modern weight management directly target the hormonal mechanisms driving the regain.
GLP-1 receptor agonists (like semaglutide and tirzepatide) work by mimicking the naturally occurring hormones that regulate appetite and blood sugar. These medications directly address the hormonal deficit created by weight loss, essentially replacing the leptin and satiety signals your body stopped producing.
According to the Centers for Disease Control and Prevention (CDC), treating obesity as a chronic disease rather than a lifestyle choice is critical. Clinical trials show these medical interventions produce sustained weight loss because they work with your biology rather than demanding superhuman willpower. They don't magically melt fat; they simply turn off the biological alarm bells, allowing you to eat normally without constant, gnawing hunger.
Lifestyle Strategies That Support Hormonal Balance
While medications are powerful tools, foundational lifestyle approaches are required to maintain a healthy hormonal environment:
The Anti-Regain Checklist:
- Prioritize Protein: High protein intake increases satiety hormones (like PYY and GLP-1) and has a high thermic effect (you burn more calories digesting it). Aim for a palm-sized portion at every meal.
- Lift Weights: Resistance training builds metabolically active muscle tissue, which helps counteract the metabolic slowdown of adaptive thermogenesis. It also heavily improves insulin sensitivity.
- Optimize Sleep: Sleep deprivation increases ghrelin (hunger) and decreases leptin (fullness), the exact opposite of what you need. Prioritize 7-9 hours nightly.
- Manage Stress: Chronic stress elevates cortisol, which promotes abdominal fat storage and worsens insulin resistance.
Redefining Success
Perhaps the most important intervention is mental: understanding that your weight regain is not a personal failure, but a predictable biological response. This knowledge can reduce the intense shame and self-blame that so often trigger vicious cycles of restriction and binge eating.
Maryland Trim Clinic (MTC) in Laurel, MD
If you are exhausted from fighting your body's set point and want a strategy based on medical science rather than sheer willpower, the Maryland Trim Clinic (MTC) in Laurel, MD, is here to help. They understand that chronic dieting damages your metabolism and skews your hormones.
Instead of handing you another restrictive meal plan, the medical professionals at MTC look under the hood. They offer comprehensive metabolic testing and analysis to see exactly how your unique metabolism is functioning. If your hunger hormones are dysregulated, they can provide advanced treatments, such as GLP-1 weight loss injections, to quiet the "food noise" in your brain. By combining these medical tools with a personalized medical weight loss program, MTC helps you achieve sustainable results by finally working in harmony with your biology.
The Bottom Line
Serial dieters are not lacking willpower. They are fighting a highly sophisticated hormonal system designed to defend body weight at all costs. Leptin drops, ghrelin spikes, insulin resistance develops, metabolism slows down, and the brain's reward systems recalibrate to make high-calorie foods irresistible.
The solution is not more restriction, more guilt, or greater discipline. The solution is working with your hormonal reality. You haven't been failing the same diet repeatedly, you have been fighting against fundamental human physiology.
Talk to healthcare providers who understand metabolic compensation. Stop trying to overcome your biology, and learn how to heal it instead.
Medical Disclaimer: The information provided in this article is for educational purposes only and does not constitute medical advice. Always consult with a qualified healthcare provider before starting any new diet, exercise routine, or medical weight loss treatment.
Frequently Asked Questions
Q: Why do I always regain weight even though I stick to my diet initially? A: Weight regain isn't about willpower, it's driven by severe hormonal changes that occur after you lose fat. Your leptin (satiety hormone) drops dramatically while ghrelin (hunger hormone) increases, creating intense, constant hunger signals. Additionally, your metabolism slows down, meaning you burn fewer calories than expected for your new body size.
Q: What is the weight 'set point' and can I change it? A: Your set point is a weight range your body actively defends through hormonal and metabolic mechanisms. When you drop below this range, your body activates hunger hormones to pull you back up. While it is very difficult to lower a set point permanently through dieting alone, medical interventions (like GLP-1 agonists) and sustained muscle-building can help shift your set point over time.
Q: Do weight loss medications actually work better than diet and exercise? A: Modern weight loss medications (like GLP-1 agonists) work by addressing the actual hormonal deficits that drive weight regain. They essentially replace the satiety signals your body stops producing after weight loss. They are not "shortcuts", they are clinical treatments for the legitimate hormonal disorder that develops after severe caloric restriction.
Q: Why am I so much hungrier after losing weight than before? A: After weight loss, ghrelin (your hunger hormone) increases by up to 24% and stays elevated, while leptin (your satiety hormone) drops to about 60% of normal levels. This combination means you feel hungrier before meals and less satisfied after eating. Your brain literally perceives food as a higher reward to trick you into eating more.
Q: Is metabolic damage from dieting permanent? A: Metabolic adaptation can persist for years after weight loss. However, it isn't necessarily permanent for everyone. Resistance training (to build metabolically active muscle), eating adequate protein, and avoiding extreme caloric restriction can help minimize or reverse some of this metabolic slowdown.
Ready to Stop the Yo-Yo Dieting Cycle?
Take Control of Your Hormonal Health Today If you are tired of fighting your biology and want a medically sound approach to weight management, expert help is available. Partner with the clinical team at MTC to build a plan that addresses the root cause of weight regain. Visit Maryland Trim Clinic to Schedule Your Consultation