Insulin Resistance & Stubborn Belly Fat: A Medical Guide

If your belly fat won't budge, insulin resistance is likely the medical reason why. You've counted calories, logged miles on the treadmill, and cut back on dessert—and yet the fat around your midsection refuses to move.
Before you blame your willpower or your metabolism, it is worth understanding what is actually happening at a hormonal level inside your body. Because for millions of adults, the real obstacle isn't discipline. It is a condition called insulin resistance—and it operates like a biological lock on your fat cells, one that no amount of cardio can simply run off.
What Insulin Resistance Is and How It Locks Fat Cells Shut
The Role of Insulin in Your Body
Insulin is a vital hormone produced by the pancreas with one primary job: to move glucose out of your bloodstream and into your cells, where it can be used for energy. Every time you eat carbohydrates—or even protein in significant amounts—your blood sugar rises, and your pancreas releases insulin in response.
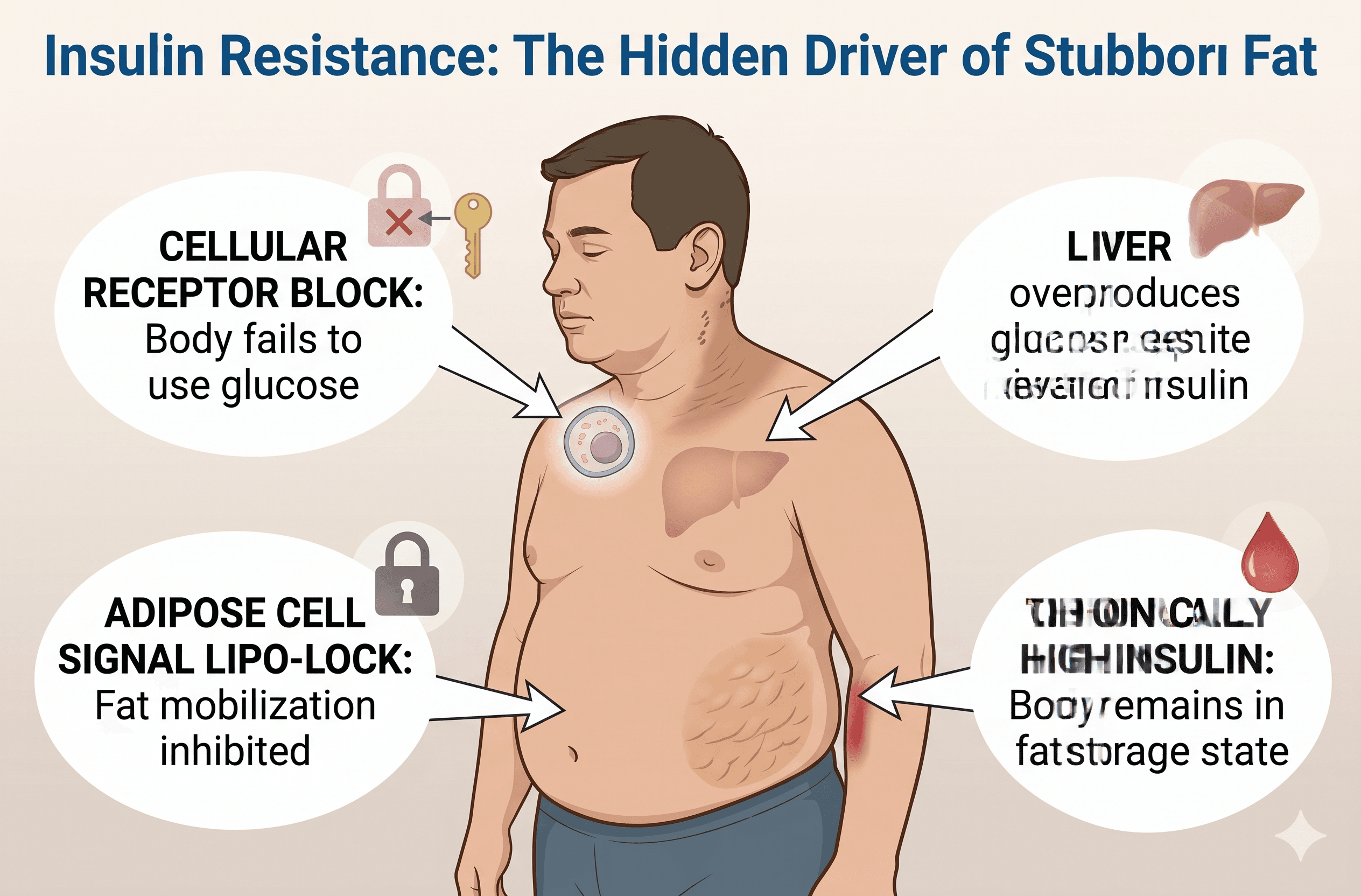
Think of insulin as a key and your cells as doors. When the key works correctly, glucose enters the cells smoothly, blood sugar normalizes, and your body returns to a fat-burning state. But here is where the problem begins.
When the Key Stops Working
Insulin resistance occurs when your cells—particularly in the liver, muscles, and fat tissue—stop responding normally to insulin's signal. The doors become stuck. According to the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK), your pancreas, sensing that blood sugar is still elevated, does the only thing it knows how to do: it produces more insulin. Over time, you end up with chronically elevated insulin levels (a condition called hyperinsulinemia), even if your blood sugar looks relatively normal on a standard test.
This is where stubborn fat enters the picture.
The Fat-Locking Mechanism
Insulin is not just a blood-sugar regulator. It is also a powerful anti-lipolytic hormone—meaning it actively suppresses fat breakdown. When insulin levels are high, a key enzyme called hormone-sensitive lipase (HSL) is inhibited. HSL is responsible for releasing stored triglycerides from fat cells so they can be burned for energy.
In simple terms: when insulin is elevated, your fat cells are biochemically locked shut.
This explains why someone with insulin resistance can be in a moderate caloric deficit and still not lose body fat. Their fat cells are receiving a continuous chemical signal that says store, don't release. The body, starved of accessible fuel, responds by slowing metabolism, increasing hunger hormones like ghrelin, and cannibalizing lean muscle tissue instead—a metabolic nightmare that makes the situation progressively worse.
Why Belly Fat Is the Epicenter
Visceral fat—the deep abdominal fat that accumulates around your organs—is not just cosmetically problematic. It is highly active tissue that both causes and worsens insulin resistance.
Visceral fat cells release inflammatory cytokines and free fatty acids directly into the portal vein, which feeds the liver. This triggers a cascade that further impairs insulin signaling, creating a self-reinforcing cycle: insulin resistance promotes visceral fat storage, and visceral fat storage deepens insulin resistance.
If you are carrying stubborn belly fat that refuses to respond to conventional dieting, there is a significant probability that insulin resistance is driving it at a physiological level.
The Foods, Habits, and Meal Timing Patterns That Worsen Insulin Resistance
Insulin resistance doesn't develop overnight. It is the cumulative result of years of dietary patterns, lifestyle habits, and environmental stressors that chronically overstimulate the insulin pathway. Understanding these drivers is critical.
Ultra-Processed Carbohydrates and Refined Sugars
The most direct driver of insulin resistance is chronic overconsumption of rapidly digestible carbohydrates. These foods spike blood glucose sharply and rapidly, demanding a massive insulin response. Over the years, the repeated high-amplitude insulin spikes desensitize cellular receptors.
Quick Swaps to Lower Insulin Spikes:
- If you eat: White bread, pasta, or sugary breakfast cereals.
- Try instead: Steel-cut oats, quinoa, or lentil-based pastas.
- Avoid: High-fructose corn syrup (found in sodas and processed condiments), which is metabolized in the liver and promotes fatty liver disease.
Sedentary Behavior
Skeletal muscle is the largest consumer of glucose in the body, responsible for up to 80% of insulin-stimulated glucose uptake. When you are sedentary, your muscles become less sensitive to insulin because they simply don't need much glucose. This forces the pancreas to secrete more insulin to achieve the same effect. Interestingly, a single bout of exercise can temporarily improve insulin sensitivity for 24–48 hours.
Poor Sleep and Chronic Stress
Just one night of poor sleep can significantly reduce insulin sensitivity. Sleep deprivation elevates cortisol and growth hormone in patterns that antagonize insulin's action.
Chronic stress has a similar effect. Elevated cortisol raises blood glucose through gluconeogenesis (glucose production in the liver), demands a corresponding insulin response, and simultaneously promotes visceral fat storage. This is the physiological mechanism behind stress-related weight gain—it is hormonal, not just behavioral.
Meal Timing and Frequency
Grazing throughout the day keeps insulin elevated for the majority of your waking hours. Insulin has no opportunity to fall to baseline levels, meaning the body spends very little time in a fat-burning state. Every time you eat a snack, you trigger an insulin response that can suppress fat breakdown for 2–4 hours.
Alcohol Consumption
Alcohol is metabolized in the liver with priority over all other fuels, effectively halting fat oxidation while it is being processed. Beyond this, alcohol disrupts sleep architecture, raises cortisol, and contributes to fatty liver—all of which compound insulin resistance.
Evidence-Based Steps to Improve Insulin Sensitivity and Unlock Stubborn Fat
The encouraging reality is that insulin resistance is not a permanent condition. It is highly responsive to targeted lifestyle interventions. The following strategies are supported by clinical research.
1. Prioritize Resistance Training Over Cardio
While cardio has cardiovascular benefits, resistance training is significantly more effective at improving insulin sensitivity long-term. Building lean muscle mass increases the body's glucose storage capacity. The Centers for Disease Control and Prevention (CDC) emphasizes muscle-strengthening activities at least two days a week for metabolic health. Aim for progressive overload to drive ongoing adaptation.
2. Implement Time-Restricted Eating
Concentrating your food intake within a defined window (e.g., 8–10 hours) gives your body an extended daily period of low insulin.
- Practical Framework: Finish eating by 7:00 PM and delay your first meal until 11:00 AM. This creates a 16-hour fasting window that allows insulin to remain suppressed overnight.
3. Restructure Carbohydrate Quality and Timing
You do not need to eliminate carbohydrates entirely, but type and timing matter.
- Prioritize low-glycemic, fiber-rich carbohydrates (legumes, non-starchy vegetables, berries).
- Consume the majority of your carbohydrates in your post-workout window, directing glucose into muscle glycogen replenishment rather than fat storage.
4. Increase Dietary Fiber and Protein
Dietary fiber slows gastric emptying and blunts the glycemic response to meals. Aim for 30–40 grams of fiber daily from whole foods. Protein powerfully suppresses hunger, preserves lean muscle mass during fat loss, and has a minimal impact on blood glucose.
5. Optimize Sleep
Targeting 7–9 hours of quality sleep per night is non-negotiable for metabolic health. Keep the bedroom cool and dark, eliminate screens 60 minutes before bed, and avoid alcohol in the evening.
6. Manage Cortisol Actively
Chronic stress management is a metabolic intervention. Evidence-based practices including mindfulness meditation, progressive muscle relaxation, and regular outdoor walks reduce cortisol levels and improve insulin sensitivity.
7. Consider Targeted Supplements (With Medical Guidance)
Several supplements have demonstrated modest but meaningful effects on insulin sensitivity, including:
- Berberine: Shown to improve fasting glucose.
- Magnesium: A cofactor in over 300 enzymatic reactions; deficiency is linked to insulin resistance.
- Myo-inositol: Particularly helpful for women with polycystic ovary syndrome (PCOS).
- Always discuss supplementation with a qualified healthcare provider.
8. Get Tested — Not Just for Blood Sugar
Standard fasting blood glucose tests often miss early-stage insulin resistance. Ask your doctor for a fasting insulin level and calculate your HOMA-IR score (a formula using fasting glucose and fasting insulin). A HOMA-IR above 2.0 suggests mild resistance; above 2.9 is considered significant.
Maryland Trim Clinic (MTC) in Laurel, MD
Overcoming insulin resistance requires personalized, clinical care rather than guesswork. The Maryland Trim Clinic (MTC) in Laurel, MD, offers comprehensive, medically supervised support for individuals struggling with stubborn fat and complex metabolic roadblocks.
Because standard blood tests often miss early insulin resistance, MTC provides advanced metabolic testing and analysis to pinpoint exactly how your body processes fuel and responds to insulin. Armed with your unique biological data, patients can participate in a customized medical weight loss program designed to safely lower insulin levels and unlock stored fat. MTC also offers expert nutritional counseling and coaching to help you build sustainable, blood-sugar-friendly eating habits, alongside advanced treatments like GLP-1 weight loss injections for those who medically qualify. By partnering with the Maryland Trim Clinic, you get a targeted, medically supervised strategy to heal your metabolism.
The Bottom Line
Stubborn belly fat is rarely a simple matter of eating less and moving more. For a significant portion of the adult population, insulin resistance is operating as a physiological barrier that makes conventional approaches ineffective. Understanding this mechanism—and systematically addressing the dietary patterns, lifestyle factors, and hormonal environment that perpetuate it—is the key to unlocking fat stores.
This is not about extreme diets or punishing exercise regimens. It is about working with your hormonal biology rather than against it. Reverse the resistance, and the fat loss follows.
Frequently Asked Questions
Q: How do I know if I have insulin resistance? A: The most reliable way is to ask your doctor for a fasting insulin blood test alongside your standard fasting glucose. These two values are used to calculate your HOMA-IR score. A score above 2.0 suggests mild resistance, and above 2.9 is considered significant. Symptoms like persistent belly fat, energy crashes after meals, and intense carbohydrate cravings are also common indicators.
Q: Can insulin resistance be reversed completely? A: Yes, in most cases insulin resistance is highly reversible, especially when addressed before it progresses to type 2 diabetes. Studies show that sustained lifestyle interventions—including resistance training, dietary modification, improved sleep, and stress management—can normalize insulin sensitivity within weeks to months.
Q: Is intermittent fasting safe for people with insulin resistance? A: For most otherwise healthy adults, time-restricted eating is safe and well-researched for improving insulin sensitivity. Allowing insulin levels to drop during fasting windows reactivates fat-burning enzymes. However, if you have type 1 diabetes, are pregnant, or are on blood sugar-lowering medications, consult your doctor first, as adjustments to medication may be necessary.
Q: Why does belly fat specifically indicate insulin resistance? A: Visceral fat is metabolically distinct from subcutaneous fat. Visceral fat cells are highly sensitive to cortisol and insulin and release inflammatory chemicals directly into the liver's blood supply. The relationship is bidirectional: insulin resistance promotes visceral fat accumulation, and visceral fat worsens insulin resistance.
Q: Do I need to cut out all carbohydrates to fix insulin resistance? A: No. A complete elimination of carbohydrates is not necessary. What matters most is the quality and context. Replacing refined, high-glycemic carbohydrates with fiber-rich, low-glycemic options significantly reduces the insulin demand per meal. Timing carbohydrates around exercise also makes a substantial difference.
Q: How long does it take to see results once you start addressing insulin resistance? A: Improvements in insulin sensitivity can begin within days of implementing consistent changes, particularly after starting an exercise program. Visible changes in body composition, especially visceral fat reduction, typically become noticeable within 8–16 weeks. Blood marker improvements often precede visible physical changes, making regular testing highly valuable.
Ready to Unlock Your Metabolic Health?
Stop fighting against your hormones. Reach out to a licensed medical weight loss clinic today to schedule a comprehensive metabolic evaluation and get a customized plan designed to target stubborn fat at the source.