Phentermine or GLP-1 Injections Which Weight Loss Option Fits You

Phentermine for Weight Loss What Patients Should Know About Safety, Eligibility, and Next Steps

Phentermine is a prescription medication that can reduce appetite and support weight loss for some people when combined with a reduced-calorie plan and lifestyle changes. If you are considering it, the most important questions are not “How fast does it work?” but “Is it safe for me?” and “What does proper monitoring look like?”
What you’ll get in this guide
- A patient-safe eligibility checklist you can use before a consult
- The most important side effects and red flags to know
- A simple decision tool to compare options (including GLP-1 programs)
- A practical next-step plan to bring to a clinic visit in Laurel, Maryland
What is phentermine and what is it not?
Phentermine is a prescription appetite suppressant used as a short-term adjunct to exercise, behavior change, and caloric restriction for certain patients with obesity or overweight plus risk factors. It is not an over-the-counter supplement, not a cosmetic “fat dissolver,” and not a stand-alone solution.
It helps some patients control hunger enough to follow a plan more consistently, which is often the real bottleneck in early weight loss.
How does phentermine work for weight loss?
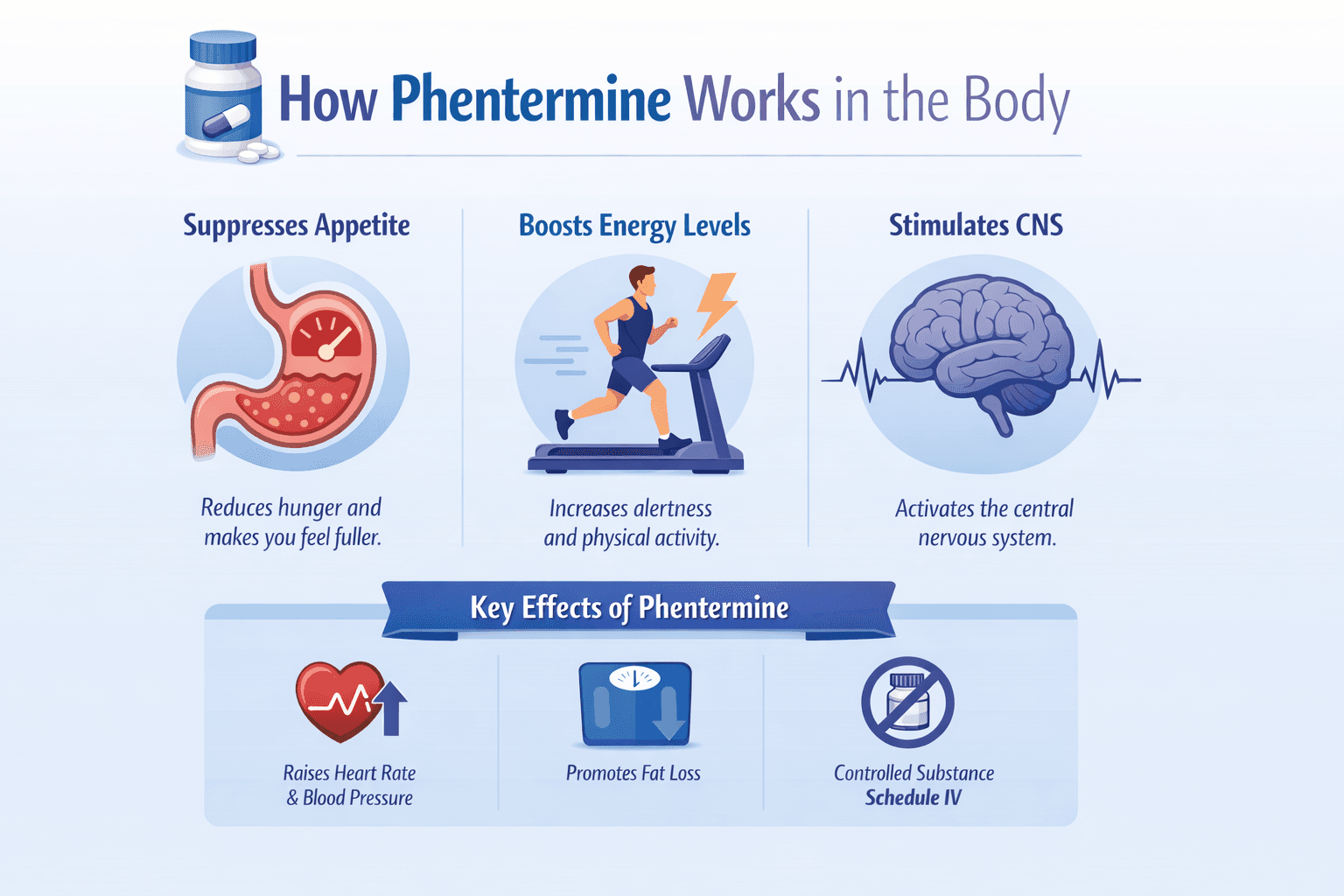
Phentermine works primarily by decreasing appetite and helping you feel less hungry or full longer. Many people also notice stimulant-like effects such as feeling more “up” or having trouble sleeping, which is why clinician guidance matters.
A useful way to think about it: phentermine may reduce the “noise” of hunger, so your nutrition and activity plan becomes easier to follow.
Who is a typical candidate for phentermine?
A typical candidate is an adult with obesity, or an adult with overweight plus certain weight-related risk factors, when diet and exercise alone have not led to enough improvement in health risks. On official labeling, it is indicated for patients with an initial BMI at or above 30, or at or above 27 with risk factors such as controlled hypertension, diabetes, or hyperlipidemia.
PHEN-SAFE Eligibility Checklist (bring this to a consult)
Use this checklist to prepare, not to self-prescribe:
- Your goals: appetite control, cravings, portion size, energy, or a structured plan
- Your medical history: blood pressure, heart conditions, thyroid disease, eye pressure/glaucoma, diabetes, kidney issues
- Your medication list: especially antidepressants and any recent MAOI use
- Your schedule: sleep, shift work, caffeine use, stress level
- Your non-negotiables: avoiding jitters, prioritizing sleep, avoiding injections, or needing frequent check-ins
Book Free Consultation Now
Who should not take phentermine?
People with certain conditions should not use phentermine, and others need extra caution and monitoring. The prescribing information lists contraindications such as history of cardiovascular disease, uncontrolled hypertension, hyperthyroidism, glaucoma, agitated states, history of drug abuse, pregnancy, and nursing. It is also contraindicated during or within 14 days of MAOI use due to risk of hypertensive crisis.
If you are pregnant, may become pregnant, or are breastfeeding, phentermine is not appropriate.
How long is phentermine usually used and why?
Phentermine is commonly prescribed short-term, and many clinicians think about it as a “jump-start” tool while habits and routines become consistent. It is often described as approved for up to 12 weeks, though some clinicians may extend use with close monitoring when appropriate.
What matters most is not a single “standard duration,” but whether benefits outweigh risks for you, and whether follow-ups are consistent.
When does phentermine start working and how do you judge progress?
Many people notice appetite suppression early, but progress should be judged by safety, adherence, and clinician follow-up, not by chasing a number on the scale. A practical, clinic-style way to judge whether the plan is working is the SAFE-START check:
SAFE-START (weekly self-check to discuss with your clinician)
- Sleep: Is insomnia increasing?
- Anxiety: Are you more jittery or restless than usual?
- Feeding plan: Are you following a realistic calorie and protein plan most days?
- Energy and movement: Are you moving more, or are side effects limiting activity?
- Signs: Any chest pain, shortness of breath, palpitations, or leg swelling?
- Tracking: Are you tracking blood pressure if you have a history of elevation?
What side effects are common and which symptoms are urgent?
Common side effects can include dry mouth, unpleasant taste, constipation, and sleep problems. Some symptoms require urgent medical advice, including chest pain, shortness of breath, swelling of the legs/ankles, and worsening ability to exercise.
Red flag rule: If you feel chest pain, significant shortness of breath, fainting, or new leg swelling, seek urgent medical evaluation.
How can you reduce side effects safely?
You can often reduce side effects by adjusting routines and getting clinician guidance rather than changing your medication on your own. Common, safer strategies to discuss with your clinician include:
- Sleep protection: prioritize a consistent bedtime, reduce late-day caffeine, and tell your clinician if insomnia appears
- Hydration and mouth comfort: frequent water intake and sugar-free options for dry mouth
- Constipation support: gradual fiber, adequate fluids, and a clinician-approved plan if needed
- Jitters/restlessness: avoid stacking stimulants (energy drinks, high caffeine) and report symptoms early
- Alcohol: ask about safety, since alcohol can worsen side effects and interactions are a concern
Can you take phentermine if you have high blood pressure or anxiety?
It depends, and this is where a clinician visit matters most. Phentermine can increase blood pressure and heart rate in some patients, and prescribing information advises caution even with mild hypertension. If you have anxiety, panic symptoms, or insomnia, stimulant-like effects may worsen symptoms and should be discussed up front.
What to ask at your consult
- What blood pressure readings make this unsafe for me?
- How often should I check BP and heart rate early on?
- What symptoms mean I should stop and call the clinic right away?
Book Free Consultation Now
Is phentermine a controlled substance and can it be addictive?
Yes, phentermine is classified as a Schedule IV controlled substance, which reflects a recognized but lower misuse potential compared with higher schedules. It can be habit-forming, and safe prescribing practices include careful follow-up, not sharing medication, and secure storage.
If you have a history of substance misuse, tell your clinician early, because that history can change which options are safest.
How long does phentermine stay in your system?
Clearance varies by person, but the mean terminal half-life is about 20 hours in labeling for phentermine-containing products. A common pharmacology rule of thumb is that it can take several half-lives for most of a drug to clear, but individual factors like kidney function and urinary pH can change this.
If you are asking this due to another medication, a procedure, or workplace testing concerns, bring that context to your clinician so you get guidance specific to your situation.
What happens when you stop phentermine?
Appetite may return, which is why the long-term plan matters more than the prescription. A strong exit strategy usually includes:
- a sustainable nutrition pattern you can repeat
- a realistic activity plan
- a follow-up schedule for accountability
- a “next option” plan if weight regain starts (program adjustments, other medications, or a different approach)
Which alternatives might be a better fit than phentermine?
Depending on your medical history and goals, other options may fit better, including structured medical weight loss programs, other prescription options, and GLP-1 injection programs that focus on appetite regulation and metabolic support. The “best” choice depends on safety, tolerability, follow-up availability, and what you can stick with.
If your biggest barrier is hunger, cravings, or inconsistent routines, medication can help. If your biggest barrier is body composition tracking, planning, or accountability, a clinic program may help even without medication changes.
How does Maryland Trim Clinic approach medical weight loss consultations?
A safe clinic approach starts with your history, current medications, and vitals, then builds a plan that matches your risks, schedule, and preferences. At Maryland Trim Clinic in Laurel, a consult should feel like a structured conversation, not a sales pitch: clarify eligibility, discuss options (including non-medication supports), and plan follow-ups.
Here are quick-start consultation prep SOP (7 steps)
- Bring your medication and supplement list
- Bring recent BP readings if you have them, or plan to have BP checked
- Write your top 3 goals (hunger, cravings, energy, health markers)
- Note sleep patterns and anxiety history
- List past weight loss attempts and what failed (time, hunger, stress)
- Bring questions about side effects and red flags
- Agree on a follow-up cadence before you start anything
To book, call (301) 960-4811 during clinic hours (Mon-Thu 9AM-5PM, Fri 9AM-1PM).
This article is educational and cannot replace medical advice for your personal situation.
Book Free Consultation Now
Frequently Asked Questions
Who can use phentermine for weight loss?
Adults with obesity, or overweight plus certain risk factors, may be candidates when lifestyle changes alone have not been enough, but eligibility is individualized. A clinician should screen for contraindications and review your medication list first.
How long does phentermine take to work?
Some people notice appetite changes early, but “working” should be judged by safety, adherence, and clinician follow-up. If side effects interfere with sleep or daily life, contact your clinician.
How long does phentermine stay in your system?
Phentermine-containing labeling reports a mean half-life of about 20 hours, but clearance varies by person. Kidney function and other factors can change how long it lasts.
Does phentermine burn fat or just suppress appetite?
Phentermine mainly supports weight loss by reducing appetite and helping you feel less hungry or full longer. Fat loss still depends on a sustained calorie deficit and a plan you can follow.
Is phentermine a controlled substance?
Yes, phentermine is classified as a Schedule IV controlled substance in the U.S. That means clinics often use safeguards like follow-ups, limited refills, and safe-storage counseling.
Can phentermine raise blood pressure?
It can, and prescribing information advises caution even with mild hypertension. If you have elevated readings or symptoms like palpitations, contact your clinician.
Can you take phentermine during pregnancy or breastfeeding?
No, phentermine is contraindicated in pregnancy and is not recommended while nursing. If pregnancy is possible, discuss contraception and timing before considering any weight-loss medication.
Can phentermine be addictive?
Phentermine can be habit-forming and is scheduled due to misuse potential, even if misuse rates are considered relatively low compared to some other controlled substances. If you have a history of substance misuse, tell your clinician early.
How long is phentermine usually prescribed?
It is commonly used short-term, and some clinicians may extend use with monitoring depending on the patient and risk profile. Ask what follow-up cadence and stop criteria your clinician uses.