The Best Diet To Follow While Using GLP-1 Medications

The Best Diet to Follow While Using GLP-1 Meds
The best diet to follow while using GLP-1 meds is a protein-first, high-fiber, minimally processed eating pattern built around smaller meals, steady hydration, and foods that are gentle on your stomach. This approach helps you keep energy up, reduce nausea and heartburn, prevent constipation, and protect muscle while your appetite is lower.
If you want one rule to start today, use this: “Protein first, plants next, and keep portions smaller.”
Medical disclaimer: This article is educational and not medical advice. Your needs depend on your health history, labs, and medications. Always follow your prescriber’s guidance.
Why diet matters on GLP-1s
GLP-1 medications and dual incretin medications (for example semaglutide and tirzepatide) can increase fullness and slow digestion, which can reduce cravings and portion sizes, but may also trigger GI side effects like nausea, vomiting, heartburn, bloating, diarrhea, and constipation, especially during dose increases.
Smaller meals and slower digestion
Because digestion slows, a large, high-fat meal can sit “heavier” and make nausea or reflux more likely. Many top pages recommend smaller meals plus planned snacks rather than one or two large meals.
Protecting muscle is part of “the best diet”
With any weight loss, you can lose some muscle along with fat. Several expert sources emphasize prioritizing adequate protein and adding strength training to help maintain lean mass.
One practical target from a JAMA patient page is: “Begin each meal with 20 to 30 g of protein.”
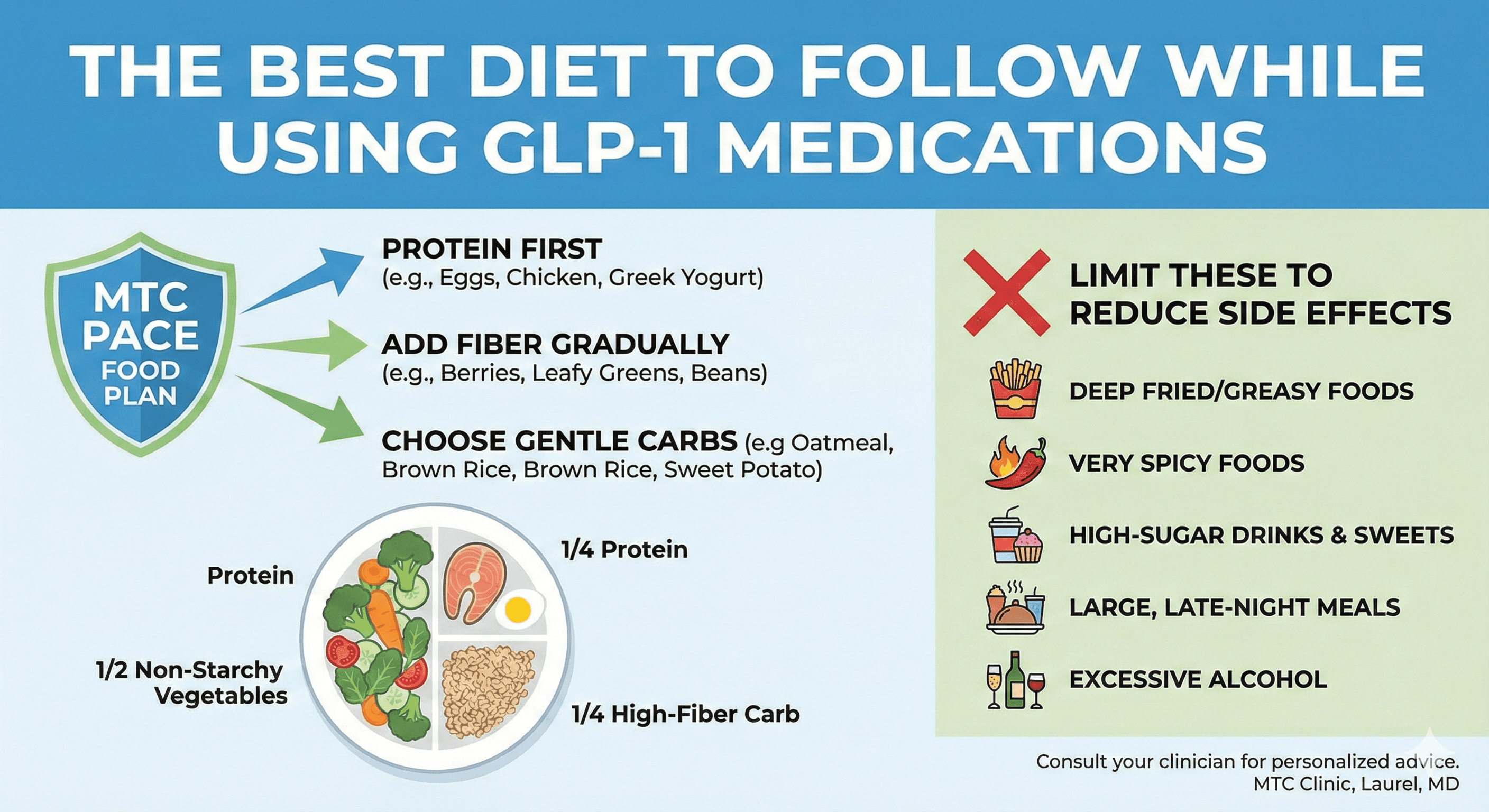
The MTC PACE food plan (simple and flexible)
This is a patient-friendly structure you can use whether you prefer Mediterranean-style eating, lower-carb eating, or a standard balanced diet.
P = Protein first
Start meals with a protein you tolerate well: eggs, Greek yogurt, fish, chicken, tofu, beans, or a protein shake if appetite is very low. JAMA suggests 20 to 30 g per meal, and also notes a daily range of 1.0 to 1.5 g/kg/day for some moderately active people, which should be individualized with your clinician.
A = Add fiber gradually
Fiber helps with constipation, but “too much too fast” can worsen gas and bloating. Build slowly, especially in the first weeks or after a dose increase. Many guidelines use about 14 g of fiber per 1,000 calories as a reference point.
C = Choose gentle carbs and whole foods
When nausea hits, bland, slowly digested carbs can help: oatmeal, whole-grain toast, rice, potatoes, bananas, applesauce. choosing slower-digested carbs and avoiding sugary drinks that can swing blood glucose.
E = Easy fats and hydration
You do not need “zero fat,” but large, greasy, high-fat meals can aggravate nausea and reflux because fat digests more slowly. Several ranking pages call this out directly.
Hydration matters too. One practical, 2 to 3 liters (8 to 12 cups) of fluid daily, mainly water, adjusted for your body size and medical conditions.
What to eat most often (with examples)
Use this as your “default grocery cart” while on GLP-1 meds.
1) Lean proteins (build every meal around one)
- Eggs, egg whites, Greek yogurt, cottage cheese
- Chicken, turkey, fish, shrimp
- Tofu, tempeh, beans, lentils, chickpeas
- Protein shakes when appetite is very low (choose options that fit your clinician’s guidance)
2) Fiber-rich plants (increase gradually)
- Berries, apples, pears
- Leafy greens, cucumbers, carrots, peppers
- Beans and lentils (start small if gas is an issue)
3) Gentle carbs for energy
- Oatmeal, whole-grain toast, brown rice, quinoa
- Potatoes or sweet potatoes
- Soups and stews for hydration plus calories when appetite is low
4) “Easier” fats in smaller amounts
- Olive oil, avocado, nuts, nut butters in measured portions
If fat worsens your nausea, use smaller servings and spread them out.
- Half plate non-starchy vegetables
- Quarter plate protein
- Quarter plate high-fiber carb
This aligns with widely used plate-method guidance (and keeps portions manageable).
Foods and drinks to limit
You do not need a “ban list,” but these often worsen side effects or derail calorie quality.
Limit when symptoms flare:
- Deep fried or greasy foods (often worsen nausea and reflux)
- Very spicy foods (can irritate reflux and nausea)
- High-sugar drinks and sweets (low satiety, can spike glucose)
- Alcohol (can worsen dehydration and GI upset; discuss safe limits with your clinician)
- Large meals late at night (reflux risk; JAMA suggests avoiding lying down for 2 to 3 hours after meals if heartburn is an issue)
Symptom-based food swaps
If you feel nauseated
- Try: Dry toast, oatmeal, broth-based soup, ginger tea, a small protein portion
- Instead of: Fried foods, heavy creamy meals, large portions
If you have heartburn or reflux
- Try: Smaller meals, baked or steamed foods, stay upright for 2–3 hours after eating
- Instead of: Late-night big meals, greasy foods
If you’re constipated
- Try: Add fiber slowly (oats, apples, beans) plus extra water
- Instead of: “All protein, no plants” days or very low fluid intake
If you have diarrhea
- Try: Bland foods, fluids, simpler meals, talk to a clinician if it persists
- Instead of: High-fat meals, large sugar loads
If your appetite is very low
- Try: Protein shake, yogurt, soup, smaller meals plus snacks
- Instead of: Skipping meals all day
A simple 1-day sample menu
This is not “the only right plan.” It is a template built for GLP-1 realities: lower appetite, smaller portions, protein first.
Breakfast
Greek yogurt plus berries, or eggs plus a slice of whole-grain toast.
Mid-morning (optional)
Protein shake or a small handful of nuts if you cannot eat much.
Lunch
Chicken or tofu salad bowl with veggies, olive oil dressing, and a small serving of brown rice or quinoa.
Afternoon snack (optional)
Apple with peanut butter, or cottage cheese.
Dinner
Baked fish or chicken, roasted vegetables, and a small serving of sweet potato.
Hydration all day
Aim toward the 2 to 3 liters (8 to 12 cups) unless your clinician has you on fluid limits.
Diet styles that usually work best
What tends to work best
A “best diet” on GLP-1 meds is usually:
- Whole, minimally processed foods
- Adequate protein and fiber
- Smaller meals plus planned snacks
This matches the common recommendations across ranking pages and clinical guidance.
Diets to be careful with
Extreme calorie restriction can worsen dehydration, fatigue, kidney problems, and nutrient gaps, especially when combined with appetite suppression.
Be cautious with:
- Crash diets and very low-calorie plans
- Aggressive fasting if you are not supervised
- Highly restrictive plans that cut major food groups without a medical reason
If you have diabetes, kidney disease, or take insulin/sulfonylureas, get clinician input before big changes.
Supplements and vitamins
Most people do best with a nutrient-dense diet rather than “auto-supplementing.” Supplements may be considered if you are at risk of deficiency (for example vitamin D, calcium, or a multivitamin), but you should decide with your clinician.
Verify checklist (bring to your next visit):
- Do I have lab evidence of a deficiency?
- Am I eating enough protein and fiber most days?
- Do I need B12, vitamin D, iron, or calcium based on my diet pattern?
Safety and when to talk to a clinician
GLP-1 and dual incretin medications have important precautions.
Do not use if contraindicated: For example, Zepbound has a boxed warning for thyroid C-cell tumors observed in rats and lists contraindication in patients with a personal or family history of medullary thyroid carcinoma or MEN2.
Wegovy’s prescribing information also includes a boxed warning and similar contraindication language.
Call your clinician promptly if you have:
- Persistent vomiting, inability to keep fluids down, or signs of dehydration
- Severe or persistent abdominal pain (ask about pancreatitis and gallbladder warnings)
- Plans for surgery or procedures requiring anesthesia (labels include anesthesia-related precautions)
Medication interactions: Zepbound’s label notes it delays gastric emptying and may affect absorption of oral medications. Share your full medication list with your prescriber.
Local note: Laurel, MD and how MTC can help (without pressure)
If you are in Laurel, Maryland, a structured plan is easier than guessing. At Maryland Trim Clinic (MTC), your clinician can review your medical history, current medications, and goals to help tailor a GLP-1 plan and the eating approach that fits your side effects and lifestyle. (Ask what nutrition support is available as part of your program.)
Book a consultation: Maryland Trim Clinic, Laurel, MD 20708, (301) 960-4811. Hours: Mon–Thu 9am–5pm, Fri 9am–1pm.
Frequently Asked Questions
1) Do I need to follow a specific named diet on GLP-1 meds?
Not usually. Many people do best with a flexible whole-food pattern that emphasizes protein, fiber, hydration, and smaller meals. That structure shows up repeatedly across clinical guidance and top-ranking pages.
2) What foods should I avoid on GLP-1 meds?
Most people do not need a hard “avoid list,” but greasy fried foods, very spicy foods, high-sugar drinks, and oversized meals commonly worsen nausea or reflux. Use your symptoms as feedback.
3) How much protein should I eat on GLP-1 meds?
A practical starting point is spreading protein across the day. One JAMA patient page recommends starting each meal with 20 to 30 g of protein and suggests a daily range of 1.0 to 1.5 g/kg/day for some moderately active people, individualized to your health status.
4) Why do I feel nauseated after certain meals?
GLP-1 meds slow digestion. High-fat, greasy meals can stay in the stomach longer and aggravate nausea or reflux. Smaller meals and simpler foods often help, especially around dose increases.
5) How do I prevent constipation on GLP-1 meds?
Increase fiber gradually and pair it with enough fluids. Several references use about 14 g fiber per 1,000 calories as a guideline, and JAMA also emphasizes adequate water intake. If constipation persists, ask your clinician about safe OTC options.
6) Can I drink alcohol while on GLP-1 meds?
Many sources recommend minimizing alcohol because it can worsen dehydration and GI symptoms and may complicate blood sugar management. Your safest answer depends on your medications and health history, so confirm with your prescriber.
7) Do GLP-1 meds cause weight loss on their own, without lifestyle changes?
In clinical trials, adding medication to lifestyle intervention produced larger average weight loss than placebo plus lifestyle alone, but individual results vary and side effects can limit adherence. For example, semaglutide 2.4 mg showed a mean change of -14.9% at 68 weeks vs -2.4% with placebo in one major trial.
8) What about tirzepatide trial results?
In a 72-week trial in adults with obesity without diabetes, the mean percentage change in weight was -15.0% (5 mg), -19.5% (10 mg), and -20.9% (15 mg) vs -3.1% with placebo. These are trial averages under study conditions, not guaranteed outcomes.
9) Do I need vitamins or supplements while on GLP-1 meds?
Often, no. A balanced diet usually covers needs better than routine supplements, but your clinician may recommend targeted supplementation based on diet pattern and labs. Ask before starting anything new.
10) Are there any people who should not take these medications?
Yes. Prescribing information includes contraindications and warnings. For example, Zepbound is contraindicated for people with a personal or family history of medullary thyroid carcinoma or MEN2. Always review your history with your prescriber.
Summary and next steps
If you want the “best diet” while using GLP-1 meds, do not chase a trendy plan. Use a protein-first, fiber-smart, hydration-supported, smaller-meal pattern and adjust based on symptoms. Bring the PACE plan and the verify checklist to your next appointment so your clinician can tailor targets to you.
If you are local to Laurel, MD, you can book a consultation with Maryland Trim Clinic to review whether GLP-1 therapy fits your medical history and how to personalize your nutrition approach.